Medically Reviewed By
Dr. Rabia Iqbal
Quick Snapshot
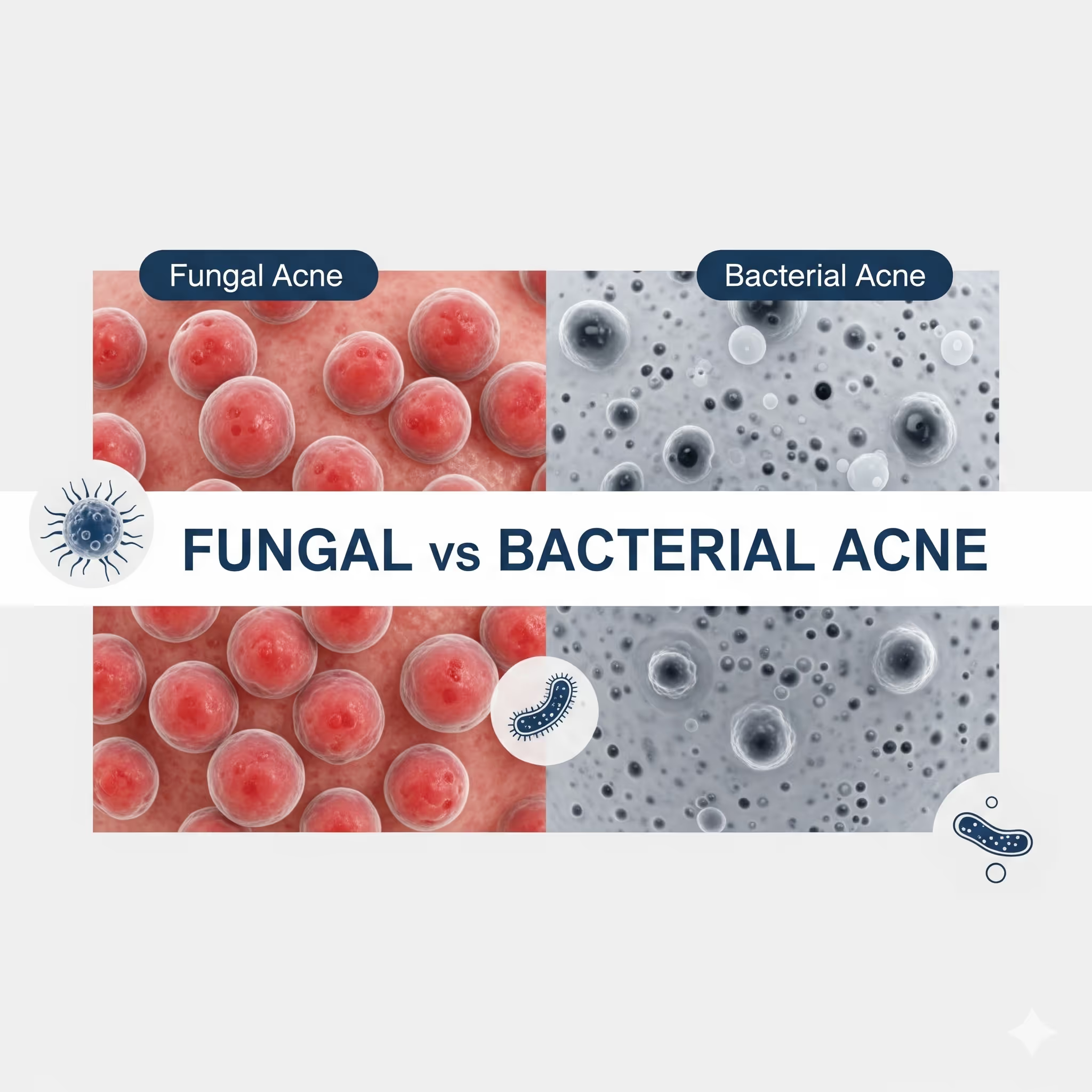
- Malassezia Folliculitis (Fungal Acne) is caused by yeast overgrowth, not bacteria; it presents as uniform, itchy, 1–2mm bumps often on the forehead, chest, and back.
- The 'Iatrogenic Paradox': Traditional acne antibiotics often trigger fungal flares by killing 'good' bacteria that normally keep yeast in check.
- Sensation is the best diagnostic clue: Fungal acne is intensely itchy (pruritus), whereas bacterial acne is typically painful or tender.
- Malassezia is 'lipid-dependent,' meaning it feeds on specific fatty acids (C11-C24); standard oils like coconut and olive oil act as fuel for the infection.
- Effective treatments include 'off-label' use of antifungal shampoos (Ketoconazole), Zinc Pyrithione, and oral antifungals for severe cases.
Causes / The Microbiome War
Fungal acne occurs due to a state called cutaneous dysbiosis—an imbalance in the skin's microscopic ecosystem. Unlike regular acne (Acne Vulgaris), which is driven by the bacterium Cutibacterium acnes and clogged pores, fungal acne is caused by Malassezia yeast.
- Antibiotic Overuse: Broad-spectrum antibiotics kill the bacteria that compete with yeast, allowing Malassezia to proliferate unchecked.
- Heat and Humidity: Yeast thrives in warm, moist environments, making this condition common in tropical climates or among athletes.
- Lipid Sensitivity: Malassezia lacks the ability to create its own fatty acids, so it 'eats' the oils (sebum) on your skin and the oils in your skincare products.
Solutions / Practical Tips — Differentiating and Treating
If you suspect your acne is fungal, follow these diagnostic and management rules:
- Check for Monomorphism. Look for uniformity. If every bump is the same size and stage of development (like a cluster of millet seeds), it is likely fungal.
- The Itch Test. If the breakout is intensely itchy or worsens with sweat, prioritize antifungal treatments over antibacterial ones.
- Audit Your Skincare. Immediately stop using products containing fatty acids with carbon chain lengths of C11 to C24. This includes coconut oil, polysorbates, and most plant esters.
- Use 'Contact Therapy'. Apply a 2% Ketoconazole shampoo (like Nizoral) as a face/body mask for 5–10 minutes daily during active flares.
- Immediate Hygiene. Shower immediately after sweating to prevent the 'greenhouse effect' that allows yeast to burrow into the follicles.
Chemistry + Lifestyle — The Fungal-Safe Protocol
- Safe Lipids: Switch to 'safe' moisturizers containing Squalane (derived from sugarcane), MCT oil (pure C8/C10), or Mineral Oil, which the yeast cannot metabolize.
- Exfoliation: Use Salicylic Acid (BHA). Because it is oil-soluble, it can penetrate the follicle to clear out the yeast and keratin buildup.
- Dietary Factors: High-sugar diets increase insulin and sebum production, indirectly feeding the yeast. Reducing refined carbs can help stabilize the skin environment.
Supplement / Product Section — Topical and Oral Support
To clear a Malassezia infection, you must reduce the fungal load while repairing the skin barrier:
- Zinc Pyrithione: Found in medicated bar soaps, this ingredient is both fungistatic and bacteriostatic, making it ideal for maintenance.
- Sulfur: A 'dual-action' hero. Sulfur works against both yeast and bacteria, making it a safe choice if you have a mixed etiology (both types of acne).
- Azelaic Acid: Excellent for clearing the dark spots (hyperpigmentation) left behind after the bumps flatten, while also inhibiting yeast growth.
- Oral Antifungals: In severe, widespread cases, a physician may prescribe Fluconazole or Itraconazole, which are secreted in sebum and kill the yeast from the inside out.
Key Benefits
Intense Itch Relief
By targeting the yeast specifically, you eliminate the inflammatory response that causes the characteristic 'maddening' itch of fungal acne.
Breaks the Antibiotic Cycle
Understanding the iatrogenic paradox allows you to stop the cycle of worsening skin caused by ineffective antibacterial prescriptions.
Microbiome Restoration
Correct treatment focuses on balance rather than eradication, helping your skin's natural flora return to a healthy, commensal state.
Chemical Literacy
Learning about C11-C24 fatty acids empowers you to choose skincare that supports your skin health rather than 'feeding' the infection.
Rapid Clearance
Fungal acne often responds dramatically to the correct antifungal treatment—sometimes clearing in 1–2 weeks after months of antibiotic failure.